Important Vocab Terms
- Tidal Volume (TV): Amount of air inhaled or exhaled with a normal breath.
- Respiratory Rate (RR): Number of breaths per minute.
- Normal Adult: 12-20 breaths/min
- Hypoxia: Low oxygen at the tissue level.
- Hypoxemia: Low oxygen in the blood (PaO₂ <80 mmHg).
- Hypercapnia: Elevated carbon dioxide level (PaCO₂ >45 mmHg).
- Oxygen Saturation (SpO₂): Percentage of hemoglobin saturated with oxygen.
- Normal: 95-100%
- COPD Normal: 88-92%
- Arterial Blood Gas (ABG): Test measuring oxygenation, ventilation, and acid base status.
- PaO₂: Partial pressure of oxygen (80-100 mmHg).
- PaCO₂: Partial pressure of carbon dioxide (35-45 mmHg).
- pH: Normal 7.35-7.45
- Atelectasis: Collapse of alveoli.
- Pneumothorax: Air in pleural space causing lung collapse.
- Pulmonary Embolism (PE): Blood clot lodged in pulmonary artery.
- Chronic Obstructive Pulmonary Disease (COPD): Progressive airflow limitation.
- Acute Respiratory Distress Syndrome (ARDS): Severe inflammatory lung injury leading to respiratory failure.
Gas Exchange Basics
Gas exchange occurs in the alveoli, tiny air sacs in the lungs surrounded by capillaries.
- Oxygen (O₂): Oxygen enters the alveoli during inhalation, diffuses across the alveolar-capillary membrane into the bloodstream, and binds to hemoglobin in red blood cells for transport to tissues.
- Carbon Dioxide (CO₂): Carbon dioxide, a waste product of cellular metabolism, diffuses from the bloodstream into the alveoli and is removed from the body during exhalation.
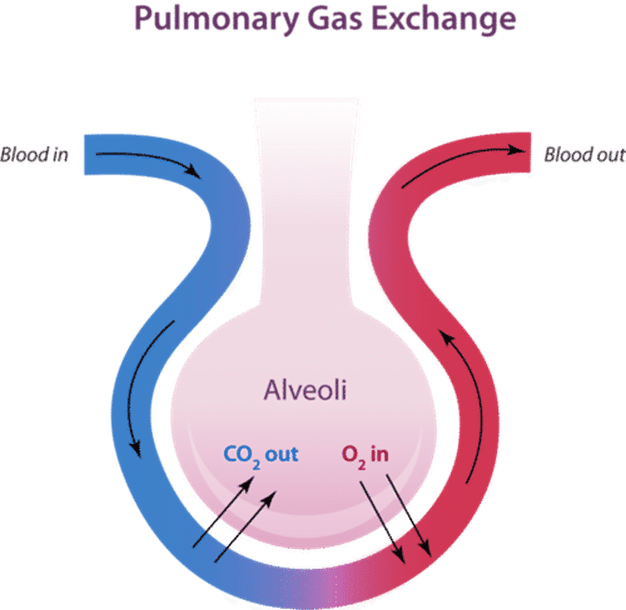
Figure A: Image showing an overview of gas exchange in the body.
High-Yield NCLEX Point: Hypoxia (Inadequate oxygen delivery to tissues) = priority problem. Low SpO₂ + respiratory distress = intervene immediately.
Oxygenation and ABG Interpretation
Here are normal arterial blood gas (ABG) values:
| Value | Normal Range |
| pH | 7.35-7.45 |
| PaCO₂ | 35-45 mmHg |
| HCO₃ | 22-26 mEq/L |
| PaO₂ | 80-100 mmHg |
- pH: Overall acid–base status
- PaCO₂: Respiratory component (controlled by lungs)
- HCO₃: Metabolic component (controlled by kidneys)
- PaO₂: Oxygenation status
Respiratory Acidosis
Respiratory acidosis is an acid-base disorder occurring when lungs cannot remove enough carbon dioxide produced by the body.
- Low pH
- High CO₂
Cause: Hypoventilation (COPD, overdose)
Respiratory Alkalosis
Respiratory alkalosis is an acid-base imbalance characterized by high blood pH and low carbon dioxide.
- High pH
- Low CO₂
Cause: Hyperventilation (anxiety, PE)
High-Yield NCLEX Point: If CO₂ abnormal → respiratory problem. If HCO₃ abnormal → metabolic problem.
Oxygen Delivery Devices
Here is a table summarizing various oxygen delivery devices:
| Device | Flow Rate | Approximate O₂ % | Notes |
| Nasal Cannula | 1-6 L/min | 24-44% | Low-flow device used for mild hypoxia. Comfortable and allows eating/talking. |
| Simple Mask | 5-10 L/min | 40-60% | Delivers moderate oxygen concentrations. Must be at least 5 L/min to prevent CO₂ rebreathing. |
| Non-Rebreather | 10-15 L/min | Up to 95% | High-concentration device with a reservoir bag. Delivers near 100% oxygen when properly fitted. |
Respiratory Illnesses
Here is a table summarizing various respiratory illnesses:
| Condition | Description | Key Symptoms | Priority Nursing Interventions | Risk Factors / Notes |
| Pneumonia | Inflammation of lung tissue due to infection. |
– Fever – Productive cough – Crackles – Dyspnea – Elevated WBC |
– Oxygen – Antibiotics – Incentive spirometer – Early ambulation |
Infection-related consolidation of lung tissue |
| COPD – Chronic Bronchitis | Long-term, irreversible obstructive lung disease characterized by chronic inflammation and mucus production. |
– Productive cough – Cyanosis – Edema |
– Low-flow oxygen – High Fowler’s position – Avoid respiratory depressants |
Often referred to as “blue bloater” |
| COPD – Emphysema | Chronic, progressive obstructive lung disease caused primarily by smoking; destruction of alveoli. |
– Prolonged expiration – Barrel chest – Thin appearance |
– Low-flow oxygen – Pursed-lip breathing – High Fowler’s position |
Often referred to as “pink puffer” |
| Asthma | Chronic inflammatory airway disease causing bronchoconstriction and reversible airway obstruction. |
– Wheezing – Dyspnea – Chest tightness – Decreased breath sounds |
– Short-acting beta agonist (rescue inhaler) – Inhaled corticosteroids – Oxygen |
Triggered by allergens, exercise, infection |
| Pulmonary Embolism (PE) | Sudden blockage in a pulmonary artery, usually from a DVT. |
– Sudden dyspnea – Chest pain – Tachycardia – Anxiety – Clear lungs – Hemoptysis |
– Oxygen – Anticoagulants – Monitor for shock |
– Immobility – Surgery – Cancer – Birth control |
| Acute Respiratory Distress Syndrome (ARDS) | Rapid-onset inflammatory lung injury causing fluid-filled alveoli and impaired gas exchange. |
– Severe hypoxemia (PaO₂ < 60 mmHg) – Refractory to oxygen – Bilateral infiltrates on chest X-ray |
– Mechanical ventilation – PEEP – Treat underlying cause |
– Often secondary to sepsis, trauma, or pneumonia |
| Pneumothorax | Air in the pleural space causing partial or complete lung collapse. |
– Sudden chest pain – Sudden dyspnea – Decreased or absent breath sounds on affected side – Possible tracheal deviation (tension pneumothorax) |
– Oxygen – Chest tube insertion – Needle decompression (if tension pneumothorax) |
– Spontaneous – Traumatic – Secondary to mechanical ventilation |
Unfamiliar Terms
- Productive Cough: Brings up mucus or phlegm from the lungs or airways.
- Crackles: Rattling lung sounds heard with a stethoscope often indicating fluid or collapsed airways.
- Cyanosis: Bluish discoloration of the skin, lips or nail beds)
- Edema: Abnormal buildup of fluid in body tissues, causing swelling. Common in legs, feet, and ankles.
- Barrel Chest: A rounded, bulging, and enlarged chest.
- Pursed Lip Breathing: A technique that helps control shortness of breath by improving oxygenation and reducing respiratory rate.
- Dyspnea: Shortness of breath.
- Short Acting Beta Agonist: “Rescue” inhaler medications that quickly relax airway muscles to treat acute asthma symptoms, COPD flare-ups, and exercise-induced bronchospasm
- Corticosteroids: Powerful anti-inflammatory and immunosuppressant medications that mimic natural cortisol to treat conditions like asthma
- Tachycardia: Resting heart rate that exceeds 100 beats per minute.
- Hemoptysis: Coughing up of blood.
- PEEP: Positive end-expiratory pressure is the pressure maintained in the lungs at the end of expiration during mechanical ventilation.
- Bilateral Infiltrates on Chest X-Ray: Indicates widespread, fluid-filled or inflamed, air spaces in both lungs.
- Refractory to Oxygen: Hypoxemia that does not improve despite supplemental oxygen.
- Severe Hypoxemia: Low oxygen in the blood (PaO₂ <60 mmHg).
Mechanical Ventilation Basics
Mechanical ventilation provides breathing support when a patient cannot adequately oxygenate or ventilate on their own. It delivers oxygen under positive pressure through an endotracheal (ET) tube.
Indications
- Respiratory Failure: Elevated CO₂ or low O₂ despite oxygen therapy
- Severe Hypoxemia: Low oxygen in the blood (PaO₂ <60 mmHg)
- Decreased Level of Consciousness (LOC): A decreased LOC with inability to protect airway
Key Priorities
- Assess breath sounds and chest rise (verify tube placement and lung expansion)
- Monitor oxygenation and ABGs
- Prevent ventilator-associated pneumonia (VAP)
- Oral care every 2-4 hours
- Elevate head of bed 30-45 degrees
- Suction as needed using sterile technique
High-Yield Respiratory Medications
Here is a table of some important respiratory medications you should be familiar with:
| Medication Class | What It Does | Example | Key Nursing Consideration |
| Short Acting Beta Agonist | Rapidly relaxes bronchial smooth muscle to open airways during acute bronchospasm. | Albuterol | Monitor HR |
| Corticosteroids | Reduce airway inflammation and suppress immune response. | Prednisone | Monitor glucose |
| Anticholinergics | Block acetylcholine to prevent bronchoconstriction and decrease mucus production. | Ipratropium | Dry mouth |
| Mucolytics | Thin and loosen respiratory secretions to improve airway clearance. | Acetylcysteine | Thin secretions |
| Anticoagulants | Prevent formation and extension of blood clots. | Heparin | Monitor bleeding |
Priority Assessment Findings
Here are the most concerning assessment findings:
- Stridor: High-pitched sound on inspiration indicating upper airway obstruction. This is an emergency.
- Absent Breath Sounds: May indicate pneumothorax, severe obstruction, or complete airway compromise.
- SpO₂ <90%: Indicates significant hypoxemia and inadequate oxygenation.
- Altered Mental Status: Restlessness, confusion, or lethargy are early signs of hypoxia.
- Use of Accessory Muscles: Neck and chest muscle retractions signal increased work of breathing and respiratory distress.
- Cyanosis: Bluish discoloration of lips or nail beds = a late and serious sign of hypoxia.
NCLEX High-Yield Point: Airway first. Airway → Breathing → Circulation (ABCs).
Image Source: “Pulmonary Gas Exchange“, by Delldot [CC BY 4.0]